
Breast cancer survivor and Best for Babes Co-Founder Danielle Rigg, JD, CLC
As a fellow double-mastectomy survivor and mom, who lost my breasts at 37, I read with tremendous sorrow Emily Wax-Thibodeaux’ story of being harassed and bullied for formula-feeding her son. Having cancer at a young age is a traumatic experience. The last thing Ms. Wax-Thibodeaux deserved was to be treated with a lack of respect or compassion.
I don’t know the specifics of where Ms. Thibodeaux delivered, or what the credentials and training of the health care professionals who tended to her were, and we have called for an investigation. But what I do know is the hurt and the grief that comes with losing your breasts during your childbearing years. I know what it feels like to be ambushed by diagnosis during the most hopeful epoch of your life and to have no choice but to sacrifice your reproductive parts to spare your whole. I know what it feels like to be betrayed by your body.
I know that the chokehold of cancer subsides as you move through surgery and treatment to recovering, but that no matter how healed you are, the pain and the fear of recurrence are ever-present. Every illness, every doctor’s visit, every peculiar lump under the skin, threatens to re-shatter your world. I know what it feels like to have your trust in statistics and your youth blown to smithereens.
I know that being pregnant and giving birth put you on a collision course with that grief all over again and that the vast majority of expecting and new mastectomies moms do not get the compassionate and evidence-based care they deserve to help them deal with the reawakening of that grief. I know that the increasing epidemic numbers of breastless young women in this country do not walk through the door of motherhood with grace, information and a full set of options.
I know that our disease-based health care system still does not properly train and educate its professionals about breastfeeding in healthy mothers — with or without breasts — because at the highest levels of policy-making we don’t value the contribution that breast milk makes to the PREVENTION of illness and to the PROTECTION of our collective health.
And I know that if I had gone on to have a third baby – mine were 2 and 5 at the time of my bilateral diagnosis – I would have wanted the journey to motherhood without breasts to have followed a very different storyline than the one presented by Ms. Thibodeaux.
I would have wanted my prenatal care provider to talk to me as both an expecting mom and a breast cancer survivor about how the birth process impacts a woman with double mastectomies; to have heard about how the delivery of the placenta triggers milk production in most mothers, so that in a very small minority of mastectomies patients, if there was any remaining mammary or nipple tissue in the armpit area, I might experience swelling in my armpits. If this was in the realm of possible for me, I would have wanted to know.
I would have wanted to hear about my options. Not just formula, but human milk-the next best substitute to milk from my own body. I would have wanted to be fully informed about the unique properties of human milk, and of the benefits and risk of milk sharing, and of the assured safety of donor milk from a HMBANA milk bank. I would have wanted to know.
I would have wanted my prenatal care provider to create a safe place for me to mourn anew the loss of a very important biological function, not just a pair of ta-tas.
I would have wanted to learn about my baby’s biological imperative to crawl from womb to breast during the magical hour after delivery, in search of comfort and food, and about how despite my new anatomy, I could still feed my child at the breast, using a supplemental nursing system (SNS) containing either donor milk or formula, and a plastic teat (nipple shield). . . I have no nipples so that would be a must. I would have wanted to know.
I would have wanted to be informed about how nuzzling and suckling skin-to-skin after birth lowers stress levels and promotes growth and enhanced food absorption in babies, and that mothers report feeling more attentive and confident one year later whether they continue breastfeeding or not.
After experiencing such catastrophic loss, every fiber of my being would have wanted to hear more about how I could still participate in this mutually beneficial and beautiful experience, and about how it might help me to heal.
I would have wanted to make an informed feeding decision and plan based on what I learned.
And when I delivered, I would have wanted my past history and my feeding plan to be well-documented in my chart, so that all hospital staff — from nurses, to feeding specialists (International Board Certified Lactation Consultants (IBCLCs)), to the pediatricians and OBs – would have been on the same page with my intention to feed this baby either donor milk or formula on my bare chest with the help of an SNS and a nipple shield. No one would have had to dig for information; I wouldn’t have had to explain. A care plan would be underway and with it, a great deal of compassionate assistance.
I would have wanted to watch my new baby crawl to my chest and be mesmerized by his motions. I would have wanted to feel him melt into me and to meet his desire for a first feed with the assistance of the professionals in the room. I would have wanted the chance for my body to nourish his, and it wouldn’t have mattered that the milk didn’t come from me. Ms. Thibodeaux was right when she took the words out of my mouth. It’s Not Just About Breastfeeding.
I never got the chance to do any of this, except in my dreams. In the 9 years since I lost my breasts, I have had a recurrent dream of birthing and nursing a new baby just this way.
If we continue the way we are going, most mastectomies moms will never get to make an informed decision or have this kind of experience, though there are a lucky few who have. Read this incredible story of a reconstructed mom who, with the help of an extraordinary IBCLC, was expertly guided from grief to alternative feeding method to profound healing and relief.
Ms. Thibodeaux didn’t get what she deserved — on many levels- and for that she has every right to be angry. But the solution is not to throw human milk and breastfeeding under the bus and with it, millions of moms and babies each year.
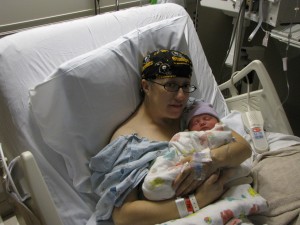
Breast cancer survivor Jamie Thomas, whose story inspired the Miracle Milk Fund, and her daughter Amelia-Rae Faith
The fact is that we need MORE not LESS systemic support for breastfeeding. Human milk does make a difference. It’s the undisputed foundation of human health and every mother’s and baby’s birthright. When you delete it from the equation of ‘how to grow a healthy human being’, there are clear population-wide negative results — including higher rates of breast cancer. It is especially a lifesaver for babies who are born early, compromised, or otherwise fragile. Read about our annual spring Miracle Milk™ Stroll and the Miracle Milk™ Fund, and take a few minutes to appreciate the staggering difference donor milk in the NICU makes in both mortality rates and suffering.
Moreover, of the 79% of new moms in this country every year who WANT to breastfeed, 60% say that they don’t make it to their personal goals of even a few days or weeks. That’s 2 million moms a year and their babies who are sabotaged by a system and a culture that do not yet get the huge emotional and physical price we all pay when women are cut off from breastfeeding.
The real bullies are everyone who tears down breastfeeding or stands in the way of helping the vast majority of moms get the information and empathetic support they need so that they and their babies can thrive, not just survive.
Fueling the argument against breastfeeding threatens to erode the impetus for that support. It throws the baby out with the bathwater. That’s the last thing all of us need.
Join the Facebook conversation on this post!
Further Reading: Why I Won’t Race for the Cure, Prevention is the New Pink, Breast Cancer Org’s: Please Include the Protection Under Our Noses, and The Cracks in the Foundation and the First Food.



WOW! THANK YOU, Danielle, for such a beautifully written, thoughtful, and fair response to Emily-Wax Thibodeaux’ story. Ever since I read her article, I have been so troubled by how to respond in a way that wouldn’t further wound her. I wanted to write something, but I didn’t. The Washington Post is my local paper. To my dismay, this week’s Health section was full of letters that unanimously praised her article and criticized breastfeeding and those of us who advocate for it. Your experience gives you unique credibility, and you write with compassion, understanding, and an appreciation for the evidence on infant feeding. Thank you, thank you, thank you! Can you please submit your article to the editors at The Washington Post? They should give your article as much attention as they did to the one by Emily Wax-Thibodeaux.
Danielle, I shared your article on my Facebook page with the following introduction: “Wow! This woman is uniquely qualified to write the very powerful, thoughtful, truthful piece below. Grateful that she took the time to respond so very well to the sad and angry article that appeared in last week’s Washington Post. I am proud of the work I do as a board certified lactation consultant and La Leche League Leader. I don’t “bully” mothers; I serve them.”
As a woman without breasts, I would not want the things that you want.
I don’t have breasts. I don’t have anything shaped like breasts. I have no idea where I would even put a nipple shield in the complicated convexities that were left after my failed reconstruction. Nor do I understand why I would bother. With nothing to latch on to, no place to put anything to latch on to, and the certainty that we’d wind up with formula anyway (because human donor milk is usually reserved for critically ill babies), I would rather go straight to formula from bottles at the beginning.
My children, like yours, were 2 and 5 when I was diagnosed. I breast fed both of them for considerable amounts of time. I also pumped, bottle fed, and gave formula - I have done all the feeding things. Were I to have another child, I would want the medical professionals who worked with me to engage with my reality. That reality would inevitably include formula, and I prefer to feed formula from bottles. I can snuggle a baby comfortably while bottle-feeding, but I was never comfortable with the SNS. I would rather lift a new infant in my arms and cuddle her close right away, than have a nurse messing around with tubing and tape while I tried to stay still for a breast crawl.
My experience of hospitals is that no matter how clear you are about something in your records, the news may not get around, particularly not to the kind of volunteer lactation consultants who suggest you might get some milk out of your armpit if you try hard enough. Those aren’t necessarily medical professionals, and don’t necessarily see patient records due to patient privacy laws. Not only would I prefer not to explain things to non-professionals who happen by, I wouldn’t want to hear “alternatives” to my proposed feeding choice, especially not stupid and impossible ones. I want doctors and nurses and everyone, frankly, to recognize that I no longer have the parts that were amputated. I’m not a starfish - they won’t grow back. I cannot “try” to breastfeed. There is nothing to work with. I prefer washing bottles to washing plastic tubing.
Elizabeth, I hear you and I wouldn’t want you to either. I’m not advocating for an SNS and nipple shield for every mastectomy survivor, I’m advocating for choice and thriving: informed decision making and quality of care - two cardinal rules of medicine that are woefully absently in maternal/infant health! There is no freedom of choice without accurate information and the support systems to carry it out. And after being down the road of breast cancer — and having been reconstructed 2.5 times, I would argue that women aren’t getting all the information there either. But our bodies have been battlegrounds over which money and politics are won for centuries….toss our boobs into the bin, and stuff us like teddy bears, we’ll deal right? Look at birth and the csection rate as another example. But I would add also that you are an aware mom, you’ve been down the breastfeeding road, and know quite a lot already about the importance of skin to skin feeding and your baby’s instinctive drive to do it that way. The same is decidedly not the experience of most women in this country — especially among minority and low-income populations. Most of America is still living in a breastfeeding desert, where health care providers don’t mention breastfeeding, let alone donor milk. If men got the kind of care for prostate cancer, or heart disease that women do for infant feeding, there would be a public outcry. The bottom line is that we can’t afford for this to continue — almost every epidemic out there would be improved with more human milk and breastfeeding. We need a prevention-based health care system that invests in training and education about human milk & facilitating the biological, physiologic, pattern of human babies and their mothers- that way we can give women and babies better care and information and let them decide what to do. I’m on the side of us all thriving.
Danielle, there are many points of concern for me in your latest post.
First: I think you overstate the availability of donor milk. It is my understanding that screened donor milk is available only to critically ill infants, and that even in those cases, it is quite expensive. If a patient will not be able to get donor milk, it makes no sense for a doctor to inform her about it. The doctors spoke to me a little about donor milk when my daughter was in the NICU (she was premature). The basic gist was that they weren’t able to give donor milk to preemies who weren’t having problems that could be specifically addressed by avoiding formula, and weren’t particularly at risk for NEC. Had I not been able to pump enough milk for my daughter (who was robust for her gestational age), I would not have hesitated to turn to formula.
It may be that many women are lacking in information about breast feeding, but I would argue that bilateral mastectomy patients who go on to have babies are not “uninformed” or “uneducated” even if they have no information about breast feeding at all. Typically, I seek information that has a chance of making a difference to me. If I knew I wasn’t going to breast feed, I wouldn’t read about breast feeding, for much the same reason that I didn’t read up on cancer treatments that weren’t relevant to the kind of disease I had.
For all either of us knows, Emily Wax-Thibodeau (the impetus for your original article, a woman who writes for the Washington Post) had thoroughly researched every feeding option possible, and went into the hospital having actively made the choice to feed her son formula from bottles. That choice would certainly make sense. If she had the conversations she says she had with lactation consultants, they weren’t informing her of anything. They were harassing her to attempt the impossible.
Skin-to-skin contact has some benefits, mostly involving temperature regulation, but this is complicated by reconstruction. Because there is no blood circulation through an implant, it will tend to be cooler than the general body temperature, and the skin over it will be cooler as well. This is potentially confusing to a newborn engaging in an instinctive behavior, and somewhat negates the temperature regulation benefits of skin-to-skin contact. Furthermore, skin-to-skin can be accomplished without many of the things you rhapsodize about - the breast crawl, “nourishing your baby from your body”, and so on. Bottles don’t interfere with it, and discussions of the benefits can be entirely separated from discussions of breast feeding.
I’m not even sure what to make of this:
But our bodies have been battlegrounds over which money and politics are won for centuries….toss our boobs into the bin, and stuff us like teddy bears, we’ll deal right?
I really hate it when people trivialize the experience of mastectomy, treatment, and reconstruction the way you have done here. I didn’t lose my breasts because I was the powerless pawn of external forces. If you’ve been through reconstruction, you know that it is nothing like stuffing a teddy bear, and that looking normal with a sweater on doesn’t mean that you’re “fine.” No reconstruction can approximate the function of the original breast, and the feelings that patients have about their results are likely to be complicated. We can’t improve medical situations for women unless we recognize women as experts in their own situations, and respect the choices they make about how they use their bodies.
Elizabeth, thank you for sharing your perspective. Just to clarify, Danielle most certainly was not trivializing the experience of mastectomy; breast cancer, a double mastectomy and reconstruction was a brutal experience for her. Danielle and Best for Babes absolutely respect the choices that women make about how they use their bodies and Best for Babes has been the pioneer in the breastfeeding movement advocating for inclusion and for supporting ALL mothers regardless of feeding choice. The purpose of Danielle’s article was simply to offer an alternative to Emily’s. It is Emily’s prerogative to find donor milk disgusting, we have a different view and are working not only to increase the availability of HMBANA donor milk for babies that need it but also to increase awareness of the benefits and risks of milk-sharing. For example, breast cancer survivor Jamie Thomas made the informed choice to feed her baby shared donor milk, see http://www.bestforbabes.org/miracle-milk-fund/ but again that is not the choice of every breast cancer survivor, and Jamie’s diagnosis and treatment timeline coinciding with pregnancy and birth informed her choice. Of course, mothers who choose to feed formula should absolutely be respected and supported and we advocate and work for better infant formula, formula feeding information, support and resources too, for example http://www.bestforbabes.org/the-babes-guide-to-bottle-feeding/. Danielle stated very, very clearly that the way Emily Wax Thibodeaux was treated was unacceptable. As for skin-to-skin, the other key benefit besides thermoregulation is oxytocin release, which is valuable to both the mother and baby, and why we recommend skin-to-skin regardless of feeding method or substance.
Assuming that Elizabeth A has a willing and cooperative partner, one possibility is for the partner to take on the role of providing skin to skin, breast crawl and suckling.
You use what you have available. If you don’t have breasts and your partner does - well then, use the partner’s breasts!
What is good for the goose is good for the gander!
I was also struck by the insinuation that Emily Wax-Thibodeau just wasn’t educated, or else she would want what Danielle would want, a simulated breastfeeding experience despite having no milk or breast tissue at all. It’s demeaning to ignore a woman’s stated decisions and reasons and question how educated she was to have made them. The part about how we need to support breastfeeding so babies can “thrive, not just survive” is not educating; that is bullying and inducing guilt.
Pingback: Another Breast Cancer Survivor on Breastfeeding BulliesBest for Babes | Marlene Dotterer, Science Fiction and Fantasy Author
Thank you for your comments Elizabeth, I could not agree more.
Pingback: A breast surgeon weighs in on breastfeeding and breast cancer survivors | Breastfeeding Medicine