 This is the 37th in a series on Booby Traps, made possible by the generous support of Motherlove Herbal Company.
This is the 37th in a series on Booby Traps, made possible by the generous support of Motherlove Herbal Company.
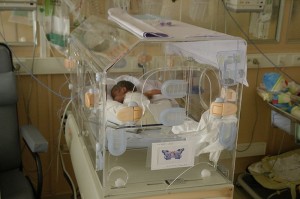
For several months I’ve been writing about Booby Traps found in the hospital for healthy, full term babies. But as we all know not all babies are born at term.
For babies born early, the importance of breastfeeding and breastmilk really can’t be overstated. Premature babies who do not receive human milk are at significantly higher risk of infections, sepsis, meningitis, digestive problems, and necrotizing enterocolitis (NEC). NEC is a life-threatening condition in which part of the baby’s intestine dies, and exclusively formula fed babies are 6 to 10 times more likely contract it than babies who receive breastmilk. All of these conditions can be life threatening to a preterm baby. Research has even found associations between breastfeeding and long term health and developmental outcomes for people born preterm.
In spite of this, parents and babies who spend time in the Neonatal Intensive Care Unit (NICU) often encounter a specific set of Booby Traps which undermine breastfeeding. I’ve listed several below, and I hope you’ll feel free to share others you have found when your babies have been in the NICU.
Not being informed of the importance of breastfeeding for a preterm baby. Given the evidence cited above, it seems unimaginable that healthcare providers wouldn’t inform a mother how breastfeeding and breastmilk could alter the life course of her infant. Unfortunately, this is sometimes the case. In Breastfeeding Answers Made Simple, Nancy Mohrbacher writes, “Where breastfeeding is not the cultural norm many healthcare providers hesitate to ask mothers to provide expressed milk for fear of putting pressure on them during a crisis or making them feel ‘guilty.'” She cites a study in which mothers of preemies who were encouraged to breastfeed stated that they didn’t feel coerced or pressured. One mother who was not informed of the importance of breastfeeding at the hospital from which she transferred stated, “I think they must have a fake license, I can’t imagine doctors and nurses do not tell mothers that there is a difference when a baby is fed their mother’s milk.” Several studies show that when mothers who had not intended to breastfeed learn of the importance of breastfeeding and breastmilk, they overwhelmingly choose to provide milk for their preterm babies, and later report being glad that they did.
Emphasis on breastmilk, but not breastfeeding. A common lament of nursing moms in the NICU is that health care providers were, “really supportive of breastmilk, but not very supportive of breastfeeding.” Mothers may hear that breastmilk is important, but get poor help establishing breastfeeding with their preterm baby - a process which is often very challenging and often requires long term, skilled assistance and support.
This doesn’t have to be the case. In Breastfeeding Answers Made Simple, Nancy Mohrbacher describes the difference between Sweden and the U.S. regarding breastfeeding in the NICU. In Sweden, “where breastfeeding is the norm, many NICUs consider parents their preterm baby’s primary caregivers and encourage them to be active in all aspects of their baby’s care. They also promote early breastfeeding as a developmental skill to be facilitated. As a result, many preterm babies are exclusively breastfeeding at much earlier gestational ages than they are in the U.S.”
In contrast, Mohrbacher writes, mothers in the U.S. “are seen primarily as providers of milk because it is widely believed that preterm babies are incapable of breastfeeding effectively. The goal is for the babies to gain enough weight to be discharged as soon as possible, and to accomplish this, bottle-feeding is often suggested. In some U.S. NICUs, expressed milk is valued as a ‘medicine’ for the baby and others efforts to express milk are a priority. In the U.S., exclusive breastfeeding of preterm babies before discharge is unusual.”
Lack of access to lactation support. The breastfeeding support needs of babies in the NICU are far greater than of the typical healthy, full term infants. Lactation consultants have a key role to play in helping mothers establish both breastfeeding and milk supply and encouraging mothers to provide milk for their babies (a function demonstrated to be wildly successful). But mothers often find that there are no or few lactation consultants to be found there. This, despite research showing that “among mothers of infants admitted to the NICU, breastfeeding rates among mothers who delivered at hospitals with an IBCLC were nearly 50% compared with 36.9% among mothers who delivered at hospitals without an IBCLC.”
Poor help establishing milk supply. Establishing a milk supply sufficient to meet a preterm baby’s needs can be very challenging, especially when the only form of stimulation comes from a breastpump. Mothers deserve expert help in this area, but many report receiving little help. This is a key support role lactation consultants can play, but as noted above, they aren’t always available.
Lack of access to donor milk. Donor milk is a lifeline to preterm babies whose mothers can’t provide them enough of their own milk. Roughly one in ten preterm babies will contract a life-threatening case of NEC (see above), and UNICEF estimates that “donor milk reduces the risk of NEC (described above) by about 79%. Donor milk also reduces the risk of late onset sepsis, another life threatening condition. The good news is that more and more hospitals are making the use of donor milk the standard of care for certain babies (often under 30 weeks gestation and weighing under 1500 grams). This means that parents at these hospitals (unless they refuse) have access to safe, life-saving human milk at the hospital’s expense. The bad news is that for too many parents, donor milk is either not used in their NICU, or if it is, they can’t get their insurance companies to cover for it. This, despite the fact that a typical baby’s use of donor milk totals a few thousand dollars and case of surgical NEC can cost up to $350,000. At $3-4 an ounce, donor milk is out of financial reach for just about all families. Neonatologists who understand the value of donor milk may try valiantly to obtain insurance coverage for it, but they are often unsuccessful. I have hope that this will change in the coming years, but for families unable to obtain donor milk now, that’s obviously of little comfort.
Poor “post discharge” support. Most parents can’t wait for the day that their baby is “sprung” from the NICU. But once home, many find that they’re treated, as far as breastfeeding goes, like any other new mom, when they require a lot more assistance. One lactation consultant I know tells me that much of her practice is devoted to desperate parents of NICU graduates who are still struggling with breastfeeding. Better follow up and coordination with community resources is needed for these families.
There are most certainly other barriers for moms of babies in the NICU, including lack of private space to pump or breastfeed, lukewarm support for skin-to-skin, and poor coordination between hospitals and providers.
There are also examples of hospitals making remarkable strides in supporting breastfeeding in the NICU, and I hope to profile one soon. In the meantime, we’d love to hear about your experiences with Booby Traps in the hospital.
Was your baby in the NICU? Did you experience any of these Booby Traps? Are there others which we’ve missed?
Image credit: Wikimedia Commons



I agree with all of these! One I would add would be a place(chair,sofa ect) to comfortably breastfeed. I had twins both in the NICU and I was never taught or helped to tandem breastfeed either…..I couldn’t imagine trying to nurse two babies in a normal chair!
My first wasn’t in the NICU, and we’re already overdue with baby #2, but I can attest to barriers with lactation consultants and the breastmilk/breastfeeding ordeal. I was so angry and upset with myself for not understanding the process, and eventually gave up after only 6 weeks with my first. The LC we had was very unhelpful and kept telling me “You’re doing it wrong” all the while not showing me what to do. How humiliating and stressful for a first-time mom just trying to do what was best. I really wish I knew the things I know now, and even though I’m still pretty unfamiliar with the process, I’m not letting them pay some person the money they do for her to be like that. I will kick the person out and have someone else come in and help us this time, and they ARE going to come check up on us this time. Last time they promised several times to do “follow-up”- which of course doesn’t happen. Sad and disgusting. No wonder so many babies don’t do well!
Amy I am so sorry for your previous experience. This time I would recommend finding a local lactation consultant from the ILCA.com website. You should have never been treated like that. If don’t know where you are located up I have a facebook page where you can post your questions and I will answer then within 24 hours. Good Luck. If I could give you some suggestions. Practice skin to skin and remember both you and your baby have the instincts of what to do.
This is the NICU at the hospital where I work to a T. No help at all, and they’re only supportive of giving pumped milk. They are also the only NICU I know of with visitor restrictions to parents! I hear so often that a baby can’t breastfeed in NICU until it can bottle feed. So not true.
My first child was induced at 37 weeks, for no good reason other than that I didn’t know any better. While he spent his time at the NICUs, the nurses dumped the colostrum I’d worked so hard to pump down the drain, right in front of me. My son’s first feeding was formula. I was heartbroken and they told me that it was my fault. I became a doula because I wanted to help other mothers get all the facts before they make birth and breastfeeding choices. If I can prevent just one mother from going through the pain I went through, I will feel like our ordeal wasn’t for nothing.
Oh, I shudder at that image of colostrum being poured down the drain right in front of you!
Good for you for turning such a heartbreaking experience into support for moms so they don’t have to experience what you did!
How is that LEGAL??? That’s YOUR milk and YOUR baby!!! This makes me so sad and angry…!
My baby had meconium aspiration and had to stay in the NICU. Due to his medical condition I was not allowed to breastfeed him right away as I had hoped. He was born at 6:29am and the hospital didn’t bring me a pump until 9:00pm even though I had been asking throughout the day if I should be pumping. When we were in the hospital we just got whatever ped from our group practice was assigned rounds that day. I was lucky the ped doing rounds the next morning was of Indian descent and encouraged me to start breastfeeding. With Dr. Achett’s “permission” the NICU nurses gave in and let me try to breastfeed my baby. By this time though, well over 24 hours after his birth and a glucose IV in his arm, my baby didn’t want to nurse AT ALL. While we were very grateful he quickly “recovered” from complications of the meconium aspiration, what kept our baby in the NICU was his refusal to breasdtfeed or even take a bottle of my pumped milk. He ended up with a feeding tube. We did the breastfeed, give a bottle of pumped milk, then the rest through the feeding tube while I pumped routine every 3 hours or less 24 hours a day everyday. I will never forget the day one of random peds doing rounds told me, “You know if you give him formula he’ll gain weight and you can go home faster.” I could feel my blood pressure skyrocket, my body shake, my fists clench, my eyes narrow. There were so many things I wanted to shout at this PEDIATRICIAN to make him realize how horrific and defeating his “advice” sounded. All I could manage was a firm, “No.” Thankfully the lactation consult at the hospital referred us to a pediatric speech therapy practice upon discharge and the women there very helpful and kind. My son FINALLY figured out the whole breastfeeding thing and we nursed until he was 17 months. He never once had a drop of formula.
I received excellent support all the way through, having had a baby at 30 weeks.. I was encouraged to express, helped to help him feed from about 33 weeks and we were discharged at 35 weeks because he was doing so well. All the nurses and doctors were very encouraging and supportive of my producing milk at home/in the comfy space provided, and then feeding him. When I worried about something, there was always someone who could come and talk with me to get me over my blip. I guess I had it somewhat easier as he was my third baby and I had breastfed the others, so I knew what to expect. Thank you to all in SCBU Gloucester (UK)..
My youngest was 10 days overdue and due with a respiratory infection that “required” him to be on IV antibiotics for 7 days in the special care nursery. He was born at home (which made him a “dirty” baby)and weighed 11 lbs. 5 oz. at birth. He nursed immediately after birth a couple of times before we transferred him to the hospital. He was on oxygen but maintained well with blow-by while I held him. As I was sitting holding my son (oh, I should mention that I am a respiratory therapist that had previously worked in a children’s hospital in the NICU), he began rooting. The nurse didn’t want me to nurse him for fear he would aspirate. Really. I told her I was going to nurse him. Period. The thing is, I was a confident 4th time mom with a medical and natural medicine background. There was so much fear in the other parents’ eyes when they would come in (occassionally) to see their children. They were at the mercy of the nurses and doctors. My dh just kind of let me run the show. But, he was in the same boat as all the other parents as far as fear. You should have seen the fear in the nurses and doctors eyes when I said I was an RT! It was fabulous!
Not all babies in NICU were pre-term. My daughter was born at 39 weeks and spent the first 4 days in NICU due to problems from labor. The biggest problem we experienced, besides those mentioned here, was the fact that I wasn’t allowed in to see her until 7 hours after she was born, and even then I wasn’t allowed to hold her until the next day. Breastfeeding wasn’t attempted until she was 20 hours old, and since it never went well (see #3-4) she was always supplemented after with my pumped milk (see #2). Other than the periods of breastfeeding every 3(ish) hours, I wasn’t allowed to be in with her. It was AWEFUL!
Thankfully we have the hang of breastfeeding now and baby is healthy and fat!
Definitely agree that the NICU my son was in had a big emphasis on breastMILK, but not breastFEEDING. There’s this whole balance of trying to help them not burn calories while they’re sucking so they’re getting the most nutrition. But once I got him home and we were able to breastfeed on our own I realized nursing wasn’t quite the workout they made it out to be. I’m sure my little guy expended more calories coughing, sputtering, and spewing from those fast-flow bottles of breastmilk they made him chug.
They are fully capable of weighing the babies before and after a feeding to find out how much they got out of a nursing session, BUT in reality the nurses may not be available to do that right at that moment, and depending on a baby’s nursing style, they may not chug down their mommy’s milk from a boobie as fast as they’re forced to from a bottle. My little guy was much more happy to rest and snuggle and nurse so that just took way too long for their 3 hour feeding schedule requirements. Even though I could tell he was nursing great (even as an inexperience first time mom) when they would “let us” have a nursing session, it would be immediately followed by them insisting I force feed him his normal amount from a bottle. It was torture so I gave up and decided to just do it their way until we got home.
Another thing that was a huge challenge is that our hospital made NO accomadations for mom. Why can’t they set up NICUs where mom can have a bed right next to baby? I lived far away from the hospital so I would get dropped off early in the morning and picked up late at night. I was absolutely beyond exhausted - there was nowhere for me to rest. Once when I looked too comfortable rocking my baby the nurse threatened to kick me out if it looked like I would fall asleep with him on my chest (Heaven forbid!)
When we left the hospital they told me I needed to give him some special formula once a day so that he got enough iron. Those first couple weeks at home I had ZERO confidence. Even though, looking back, I was making milk like a champ, I could never tell. I would feed him in the night, be afraid he didn’t get enough, get up and make him a bottle, pump to make up for the bottle that I gave him so I wouldn’t lose my precious milk supply, and by that time he’d be awake and ready to nurse again. Again - exhausted! They drilled this mandatory 3 hour schedule thing in my worried mom head so that I thought there was something wrong when my baby would nurse a bit and fall asleep at the breast. (“He didn’t get a good feeding! He’s lethargic! He must not be getting enough calories! I better give him that formula or a bottle of breastmilk because he just must not be getting enough nutrition from ME!”)
I know it’s a hard situation. The NICU nurses do their best, and they have their proven routines to fatten up these babies and send ’em home. I guess my biggest suggestion would be to break down the barriers between the mommies and their babies. Give us a room where we can lay in bed and snuggle with our babies and all their equipment so that we can actually recover, our bodies can make milk, and these little guys can benefit from REAL kangaroo care, not just their token little snippets of it once or twice a day. Even if we’re all in one big NICU all together with curtain partitions so the nurses don’t have to run all over the hospital when monitors go off, that would be better than being forced to leave your baby and have your confidence go down the tube when it seems like these nurses know everything and you know nothing.
Preemies are not only small but are notorious for being poor weight gainers. Nature somehow knows this - did you know that breast milk from a preemie mom is higher in fat content than full-term moms? (Breastfeeding is so cool.)
I had a 29 weeker in the NICU, and your list is definitely accurate! Private space to pump is a big obstacle. But I’d say learning how to establish your own milk supply is where support is lacking most of all. So many preemie moms give up too easily and too soon. Your really have to pump RELIGIOUSLY - as if your baby were home with you already. In other words, every 3 hours, round the clock. Period. No exceptions. (Fenugreek can help, too.)
One more tip - a nipple shield is a life saver for a preemie with a poor latch. My baby never learned to nurse without one, so it was a life saver for us.
My daughter was only in the NICU for two days, but we didn’t get a ton of support for breastfeeding. But then we didn’t really get discouragement either, feeding wasn’t much mentioned. I was told that I wouldn’t be able to nurse her right away, but nobody could tell me why. So I pumped and took the colostrum to her. The afternoon after she was born, I was doing kangaroo care and she started rooting like crazy. I still hadn’t been told why I couldn’t nurse her, so I said screw it and gave her the boob. She latched on and nursed like a pro.
It’s just astounding to me to hear that “feeding wasn’t much mentioned” during your daughter’s (blessedly short) stay in the NICU. There is so much evidence that feeding matters *a lot* that it just seems unbelievable that any NICU wouldn’t actively promote breastfeeding.
All of the above. I had 34.5 week twins via c-section 100 miles from home and our NICU experience was horrible. They were fine with me pumping and bringing milk in for my babies. We only had one nurse who even tried to help me put the kids to breast. We saw her twice in 10 days and the only thing she did was offer a nipple shield so my son even attempt to latch. We found out 3 weeks later he was tongue tied. I think my biggest complaint was their scheduled feedings. My milk didn’t come into until day 5 and I was okay at the time with supplementing with formula as needed. I knew that I would figure out the breastfeeding thing myself once I got home and had access to my IBCLC and peer counselor. They were determined to only feed the kids at 12, 3, 6, and 9 and they didn’t care if it was breastmilk or formula in the bottles. Now we all know that bm digests easier and they might want to eat sooner but that was not allowed. By the time feeding time came the kids were starved, upset and would cry themselves to sleep or wouldn’t want to eat at all. Or they would end up with formula in their bottle for a feed and not finish it all. It was a horrible catch 22. On day 8 we were told they had to have 24 straight hours of complete feeds in order to go home. Once we found that out we made sure we were there for every single feed with the privacy curtain up. If the kids didn’t finish their bottle we would dump the rest in the garbage. We left the hospital on day 10. It took me a bit to get the kids actively nursing and my milk production up. I ended up getting my sons tongue clipped and using a SNS for a few weeks. But by week 7 I had the kids off all supplemental formula and they were 100% breastfed.
I agree wholeheartedly with this list!!! My 37 weeker ended up in the nicu for a week. The hospital definitely promoted breastmilk over breastfeeding, which is so difficult to keep up with long term. The other issue is that you are cut off from all of your supports as they limit who can come in and your access to information while you are there. (no phones, computers, ect). I asked the nurses for help from the IBCLC on staff and was told that she was busy with babies who were about to be released and was handed a nipple shield. I never saw either of the IBCLCs in the nicu. The nicu should have a IBCLC on staff for just the nicu babies since they have such intensive needs. I could never get my milk up to the point that I didn’t have to supplement.
I had a 34 weeker and these were all so true. Sadly going back to monthly NICU reunions I would be the only one successfully breastfeeding at home. Thankfully I fought for support and ended up nursing my daughter for 4 years!
My baby was taken to the nicu for “precautionary observation” (cya). Although I had requested no formula both verbally and in writing, they told my husband it was “required” and gave him formula without my consent, without telling me or giving me the chance to express colostrum. I fought to be given permission to breastfeed for his next “scheduled feeding.” When I got there he nurse out up a screen and left. No help. In fact every time I was nursing when a nurse came in they would promptly leave like they were embarassed to have walked in on me.
My daughter was in the NICU for 5 weeks. The hospital was very supportive of breastfeeding when she was ready. I requested a pump shortly after she was born so I could pump milk for her. The nurses were great and I also got wonderful support from the lactation consultants. She didn’t start to nurse (without me pumping) until about after a month after she came home. I think part of it was due to her being premature and she just needed to have enough stamina to be able to nurse well. The nurses in the NICU told me preemies nurse better than full term babies. I guess this might be true? It worked out for us and I am so glad it did! I think the keys to success are pumping (every 2 to 3 hours) in the beginging and having the confidence that you can do it. Sometimes there are road blocks but if you get the right support it will happen! I also went for a lactaion consult after she came home to see how much she was transfering. Not much at the time but she got better shortly after and I haven’t had to use the pump for 4 months now. She is 6 months and doing wonderful! The best part about pumping for her in the begining is I have lots of frozen milk that I can now use in her cereal she has started eating. Get good support to get over the road blocks and beat the booby traps! Breastfeeding is a wonderful thing.
I could write alot about this, but won’t - I’m a NICU RN and had 2 preemies myself, but they weren’t in the NICU I work in. The NICU my boys were in asked me to write down meds I’d taken while pumping (like pain relief meds after C-S) - well first time around I did this, second time around - nope - “my” NICU gives the babies milk and don’t ask moms to write down the meds so I said forget this. But seriously - do they toss it? And I had also heard discussions about tossing a mother’s milk because she was sick - that would be great milk to pass on with all sorts of immunity in it. Another thing that was difficult - staying on a strict schedule is frustrating for some, but when you have to pump every 3 hours, it’s nice for your child to be used to eating every 3 hours and helps you plan when to visit if you can’t spend all day (because you have another child). The NICU my boys were in - got them on a feeding schedule where they would feed every 2-5 hours depending on when my child woke. Well, this made it difficult to breastfeed because I missed feeds since they were random. And they gave my 7 day old, 3 oz. at one feeding - that is way too much, but they pumped it in so he’d sleep longer. But I do agree, we in NICUs could do so much better with help with actual breastfeeding.
My twins were in the nicu-one for 48 hours and one for q week. They one in for a week had a feeding tube and had difficulty nursing. He nursed for 16 months and honestly, he really never was great at it. He decided st 16 months he wanted nothing to do with it anymore. The one in for two days was a champ from the get-go. He latched right on as soon as I was able to see him and never needed a feeding tube, though I had to pump and supplement with a bottle for two weeks until he was strong enough to exclusivelynnurse. He is still happily nursing at 20 months :). I had great support. The nurses had me try to latch immediately. One did, one didn’t. Ine came out of the nicu and roomed in withmme, one stayed. That was such a difficult juggle, but everyone worked with me and it was great. I have no complaints about our nicu time, we had a life threatening placenta situation (vasa previa), so just getting them here safely was such a relief at that point, it was hard to complain about much.
Just s funny aside- my weak nurser never ever figured out how to take a bottle. If I ever left him, I had to be back in two hours to nurse him. He just cldnt do it, it was pitiful. So, it’s definitely not always true that they have to bottle feed before breastfeed. My guy never got that one down at all.
I don’t have a personal experience to share, but I thought this article was really interesting. It sound like there is a lot that can be done to help moms of preemies get a better start with breastfeeding. I stopped by because I just read an article published last week on the effects of listening to relaxing audio recordings and seeing photos of your baby on pumped milk production in the NICU. The study showed a striking effect of this simple intervention, which makes me think that supporting moms and encouraging them to get relaxed during pumping (and providing them a comfortable place to do it) could have a real impact on milk production and establishing supply. Anyway, I wrote a blog post about the study if you are interested: http://scienceofmom.com/2012/04/12/pump-up-the-music-improving-breast-milk-production-in-the-nicu/
My son had a fever after birth so to the NICU he went. On day 3 he had lost a total of 10 oz. Sounds like a lot, especially when most of the babies TOTAL weight wasn’t much more than that in the NICU! However, his birthweight was 10 1/2 lbs! So I went into the room with the doc’s and nurses and when they started to have a fit about his weightloss, I calmly stood up. I asked the doctor what is the normal % of weightloss expected. . . 10%. And my babies was within that amount. . . . yes. He did get a bit of formula, but they stopped fussing about his weight. Sigh.
Oh, and don’t forget. . . that baby is THEIR baby until it goes home and they will do whatever they feel is necessary, permission or not. (Visitor’s aren’t allowed to sleep in the NICU, only 1 chair permitted in the NICU, no privacy for pumping or nursing in the NICU, etc.) It is the parents’ who are interupting the flow/plan, etc. Very hard to deal with for a new parent, especially if the mom had a c-section.
We had our preemie at 31 weeks and the hospital did a great job while we were there. As others have stated there was not a lot of concentration on breastfeeding, mostly on pumping. I needed that help at the time because I did not expect to be in that emergency situation. It is vital to receive support - a great percentage of women who deliver early do so because The MOM is the one sick. The consultant who helped us was awesome- to the point that I think If I had to ask to pump me herself I think she would have. She basically taught my husband how to pump for me. I was too sick to think. I would REALLY have used post hospital discharge help. It was by God’s grace that she nursed at all - I mean she would try but then fall asleep. I had my breast in-her-face constantly in case some might accidentally fall into her. She needed EVERY calorie. We brought her home at 4 lbs. She is now a thriving 10 year old.
Thank you so much for bringing this important issue to light. There is not nearly enough awareness about the lack of breastfeeding support in the NICU. I’ve had several moms voicing their concerns about this, and as the mom of a preemie myself, I can relate. Breastfeeding is even MORE important to preterm and sick newborns and not nearly enough is being done to educate nursing & medical staff on how to support anxious new mothers of babies stuck in the NICU.
In Ontario hospitals, the staff is very clear on their preference for breastmilk in most cases, and you can see tired mothers lugging jugs of their milk to the NICU fridge for storage. It’s a lot of work for these poor mothers and they do a great job. But, as you pointed out, it is so true that they receive neither adequate help learning how to breastfeed their vulnerable children nor the support they deserve once they go home.
One frequent complaint I have heard is that mothers are not given the kind of access they want to their babies. The highly regulated environment of the NICU often does not allow for the intense skin-to-skin contact mothers and babies could benefit from on a more regular basis. This, of course would also facilitate better breastfeeding.
It seems there should be a qualified lactation consultant who has special training with preterm and sick newborns on staff for every NICU. In Canada this is likely a pipe dream with the way our funding goes, but it really would go a very long way toward healthier babies and mamas.
I can relate. Our twins were born at 32 weeks and I got so much crap for insisting on breastmilk. The nurses acted as if I was trying to starve my children who had marble sized stomachs. The first day I was “allowed to put my daughter to breast” they turned me away because she has just had a hard time getting an IV….imagine what a comfort I could/should have been. We ended up getting allowed donor milk while we waited on my supply (we contemplated smuggling in milk from my sister-in-law). Thankfully we overcame and met our goals…exclusive breast milk for the first 6 months and nurawd into their 2nd year…my son weaned at 21 months and my daughter is still at oit at 24 months.
What I’d like to see is hospital LCs with preemie experience. At our hospital, the NICU nurses were honestly way more helpful than the LCs on site - who treated all of our issues like they would with a full-term baby. I had the same probably with the one private LC we saw… her solutions were the same whether your baby was born at 40 weeks or at 34 or earlier. Luckily, things worked out in the end for us - we nursed for 18 months until P. self-weaned mostly because of the NICU nurses at the very beginning and our own determination. Looking back, I’m still pretty mad at some of those LCs and their one-size-fits-all solutions!
I have had 3 late term preemies in the nicu. After reading this I am SUPER thankful that I delivered where I did! While I faced a few of these challenges with my first NICU baby, I faced none with my 2 youngest. There are wonderful IBCLC that worked with me. There was a hospital grade pump AND all the necessary supplies (including dish soap) in my postpartum room when I arrived (with all 3 births). I saw the lactation consultant by the day after I delivered. My 2nd baby was allowed to go straight to breast even before bottle feeding! And there was a pumping room in the nicu and recliners available for use while breastfeeding! All 3 of my babies came home EBF…my littlest is only a month old now but my 2nd nicu baby was EBF for 14 months. I am so thankful for the experience I had!
My son was 30weeker he was born at Dallas baylor much it was the best they told me all about breast deed and that aha I did cause that was best for him even though I was against it they told me Ho important it was for him this is the best much around even though my baby ended up have a teach and all they where very good with him. I love that hospital
Sorry my spell. Bad baby I arms baylor in Dallas is the best my son should have by lived but they saved him
I had a 29 week micropreemie. Our NICU strongly encouraged breastfeeding or rather as in #2 above, breastmilk. I had no issues with supply. In fact, I had ample supply and that was part of my problem. At 4 weeks old, he was doing great and we were just waiting on him to learn to feed. When we did starting trying, milk would let down as soon as he got on the breast and then it would just be a river of uncontrollable milk and usually from both sides at the same time. We even tried nipple shields to help him latch but the amount of milk just made it hard. Finally, one of our sweet night nurses advised us to give him a bottle (of breastmilk) and get him eating good so we could go home. She had a similar experience with her daughter, though not as early. She said once they got home and got “comfortable” together then the breastfeeding came naturally. That is what we did and at around the time of his due date, 3 weeks after going home, he finally got the hang of it. Best advice we could have gotten. We were just ready to get out of that hospital and be home.
Ironically around his first birthday , we found out he was tongue-tied severely. Two neonatologists, several NPs, all the nurses and therapists missed this. The oral surgeon who corrected it said that it likely interferred with his breastfeeding because it restricted his ability to get the correct latch. I guess my ample flow made up for that part.
Our NICU had a lactation consultant although almost all the nurses were pretty adamant about it anyway. Privacy could have been an issue for some. The NICU was just a large room for about maybe 20 babies and you could pull curtains between the isolettes which the nurses were happy to do for me when it was time to pump. They would also keep my water bottle filled for me and kangaroo care was strongly encouraged by most of them.
I had triplets at 25weeks 5 days…went spent 9 1/2 months in the NICU wih one of my daughters and 4 months with the other two. At our hospital the lactation nurses and NICU nurses were phenomenal. We tried and tried to breast feed the two that only spent 4 months but they aspirated at the breast and it became way too stressful for me. The LCs were so encouraging, never made me feel guilty, just cheered me on. Even my daughter who was the sickest (she died at 14 months), latched for 10 minutes one time. Our situation was not the norm, with micro preemie triplets and while I wish I could have breasted them all it just wasn’t possible…believe me we tried everything and even the LCs got creative! But they also respected me when I chose to kangaroo, pump and bottle feed. There were so many ways I felt like a failure as a mother during this time, but those awesome LCs never contributed to that feeling…quite the opposite. Our NICU did have comfortable recliner chairs, pumps available at all times and almost private rooms. I wish everyone could have the experience we had…at least if you are under the very challenging circumstances we were.
My son was 2 weeks late and was with me the first day. We were doing fine establishing a nursing relationship. He went into the NICU about 20 hours after he was born because they thought he might be having seizures (thankfully he was not). I was not allowed to breastfeed because he was not allowed to eat anything while they ruled out allergies.
That took 24 hours. After that time was up and before I knew that time was up, they gave him frickin FORMULA. I was upset but still didn’t know a whole lot so I wasn’t too mad, my baby was hungry. I explained that I did not want him to have anymore formula. I said I would come down every 3 hours and feed him. If he was hungry before then they were to call me down.
I had had a c section and the NICU was about a 7-8 minute walk from L&D (don’t ask me why). I woke up at midnight that night to walk down to feed my son. After a painful, long walk to the NICU I walk in to see a nurse finishing up feeding my baby a bottle of formula. I LOST MY MIND all over that place. I still attempted to breastfeed, but of course he was full.
At the very least he was not given another bottle before I was called down or attempted to breastfeed, but the damage was done. He was already to the instant gratification of the bottle and I still wasn’t producing milk so there was no comparison. FINALLY, after another 2 days, an amazing nurse (not LC but just a wonderful woman who understood how important this was) set me up with a SNS which helped bring in my milk and we got him almost completely off the formula before we left the hospital. The LCs were virtually no help once he was in the NICU except to bring me a pump and sell me a pump (which was covered since he was in the NICU, the one silver lining).
2 years later I am still angry about the formula and still tell everyone how amazing Stacey was with me and that she saved breastfeeding. It would be so different now that I know what I know, but in my new mom, baby in the NICU fog Stacey was an angel.
My son was born at 24 weeks and in the NICU for four months. Though I loved my son’s doctors, nurses, RTs, etc., (after all, they were responsible for saving his life and keeping him alive), there was absolutely no support for breastfeeding and no emphasis put on breastmilk. It was never discussed. My milk never came in. I think if anyone had taken time to discuss with me how I might be able to stimulate milk production, I would have absolutely done it, even when I was an emotional basket case, not knowing if my son would live or die. I greatly regret that I was unable to nurse or provide breastmilk for my son.
Some hospitals are getting better. Our baby was full-term and roomed in with us for two nights before the pediatrician found that she had suffered a huge fetal-maternal transfusion in utero and was severely anemic. She ended up spending six days in NICU. While I do wish they had caught her issue earlier, we had the benefits of getting started breastfeeding together and that was fabulous.
The hospital I delivered at has a reputation for being one of the best breastfeeding hospitals in the country and this extended to the NICU as well. They did keep us on a strict three hour feeding schedule, but all the NICU nurses were my personal breast feeding cheerleaders. Before I was allowed to feed her, they treated my expressed milk like liquid gold and always made a huge fuss over how much I was able to pump. They also practiced early colostrum intervention. Once feedings were allowed, they weighed her before and after and were super encouraging (“Yay! A whole ounce! That’s awesome!”). And they always gave us lots of privacy and often let us cheat and feed for longer than the official 30 minutes. This was just the regular nurses, not the lactation consultants, who were of course universally awesome.
Granted, my baby was not as sick as a lot of NICU babies and had had a chance to get the hang of things with me before we were separated. But just a positive note to say that there is hope and things are getting better. (I delivered at Brookwood in Birmingham, AL.)
I am a mom of 5 preemies, all singletons. I advocate extensively for breastfeeding moms in the NICU. It can be really really hard (sometimes almost impossible) for moms to get help getting a baby on the breast.
Many NICU nurses are much more comfortable seeing the volume a baby is taking. Also they often do not have the training or skills to help get a baby on the breast.
One mom I worked with recently, has a baby in the NICU and she was told that baby could not breastfeed because baby was cold- the baby was only in a onesie and and a single blanket- left in an open crib.
I have three preemies and could not agree more! My first was born at 33 weeks, and she was 100 miles away from where we lived-so i decided to live at the hospital. Apparently that isn’t the “norm” bc they were not equipped for me to do that and honestly, it sucked, but well worth it. She was there for three weeks, all of which I was there for-and bc I was inexperienced, I pumped, but she never got breastfeeding and went home on a bottle bc the nurses kept pushing bottles and that we could work on breastfeeding at home).The nurses kept telling me she would come home faster if she took a bottle, so that is what i did. I was told all the benefits of BREASTMILK but not breastfeeding. Since I was not given the knowledge of how to nurse a preemie, we never got the hang of it …But I made the decision to pump for her for 14 months, and she never had formula-it is possible!!! My next two were twins born at 32 weeks, and were transferred 100
miles away from where I was in the hospital (i didn’t get to see them until 4 days after they were born, but started pumping right away) I told the doctors and nurses right away that I wasn’t going home with my babies until they both could nurse exclusively…and many fought me all the way. But I was determined bc i knew i would never figure it out on my own, at home with twins! I had a nurse who was in my side, she fought for and with me! And i did it, they came home 5.5 weeks after their birth, both on the same day and only nursing! I was told I was a minority,in fact they didnt know of any other set of twins that had done both of those before! Most dont come home together and never exclusively nursing! I lived at the hospital full time the last week and a half before they came home, just to work on nursing and it was worth it. They are now almost 5 moths old and haven’t had formula! More knowledge (and perhaps pushing) of breastfeeding needs to be done in NICU’s!
Most of ours nurses were great, as were the facilities, the second time! We had a privite rooom, a pump in the room and supplies, including dish soap, plus more support overall from the hospital! We loved Children’s Hospital in Minneapolis, MN!
I have a great hospital… from my experience, this list doesn’t really apply. I have a free boarding room to stay in just upstairs from the NICU so I have a private space to sleep, shower, pump, etc. The SCN has comfy rocking chairs, curtains to pull around your area for privacy, and wonderful nurses and LCs who are helpful and encouraging. But despite all this I couldn’t nurse at all. I have major supply issues due to IGT so I was prepared with More Milk Plus, Goats Rue, Go Lacta and placenta capsules, and an SNS for supplementing with donor milk if needed… but my baby was born with no thyroid gland and was in pretty rough shape. He was on CPAP and IVs and under the bilirubin lights. I couldn’t even hold him for several days. Once I could hold him, they let me put him to breast but all he did was lick me a few times and sleep. He slept almost all the time and was never hungry. He finally perked up after 2 weeks when his thyroid meds took effect. He began to root and want to suck. But my milk had already dried up before he was one week old. Those first six days I had taken my supplements, drank tons of water, pumped religiously every 2 hours. The most I ever got out was 3/4 oz combined for one time.. 2 hours later it was 1/4 oz, and then it was down to a couple ml at a time until it was gone. But they gave every drop to him through his tube, and never made me feel bad. Since my milk’s been gone, he’s been getting hospital donor milk. We’ve been here 6 weeks now (he was 37 weeks at birth) and we still have probabably at least 2 more weeks to go… it’s been a long haul but I’m so glad we’re at such a great hospital!
Wow what an incredible story. Our hats are off to you for everything you’ve endured and we have the greatest admiration for your efforts to manage your IGT and give your baby your pumped milk and donor milk. Your son is lucky to have an amazing mama!
I just went through this myself. This being my 9th child (having breastfed all previous ones too), I knew what I wanted and I knew what was best for my child. My son was born 4 weeks early and was really in great shape; but they whisked him off to the NICU right off the bat and complained about his blood sugar levels, bilirubin, you name it. All within recommended AAP levels; but somehow not “good enough” for release. Right off the bat I got an attitude because I would not allow them to give him pacifiers or bottles. I had a previous child who was given a bottle in the hospital and it completely messed up our breastfeeding…from that point on he would not nurse unless my milk was actively letting down; I only nursed him a month before I gave up in frustration. For those going through this, THERE IS ANOTHER OPTION… a gavache (feeding tube). This does not mess up their suck or cause nipple confusion, and you can pump and they will give them the breastmilk this way. Even though my son was plenty old enough to drink from a bottle, I wanted to preserve our nursing relationship since it is so critical to preemie babies. Unfortunately, plan to eventually have a requirement of 24 to 48 hours of complete oral feedings before release.
The second nightmare: Although the hospital was great about offering pumping rooms, privacy and whatnot, the whole scheduled feeding thing was a nightmare. They required 2 ounces of food every 3 hours; naturally he was given formula since I didn’t have all that milk initially. Really, the only days I was able to keep up with their “schedule” was, thankfully, the day before he was released when I was gorged from fresh milk supply (it was very slow to come in with all the stress). I knew he just needed to sleep in a 4, 5 hour block; that he would wake up hungry and eat a load and continue to cluster feed. But they would not allow this; I was forced to go by their schedule, even when they allowed him to eat MORE often. It was so frustrating. The weighing of him before and after was stressful, the breastfeeding became WORK, and I learned every trick in the trade to keep him awake to get those ounces in him. I was successful, thankfully… but the last night I had to give in and allow them to give him a bottle with a slow flow… just so they could release him. I was in tears, the next day he was latching odd (thankfully just for a feeding or two), and I got to go home!
The frustrating thing about all this is that he was gaining just short of an ounce a day in the hospital. In the three days that we were home he gained TWO OUNCES a day, double the average; even though he went for larger blocks of sleep, etc… As a mom it’s so frustrating to not be able to do the best by your child, to lose your parental rights in that way.
Pingback: Booby Traps Series: How to beat the Booby Traps in the NICU. An interview with Diane Spatz. | Best for BabesBest for Babes
Pingback: FAST FACTS: Miracle Milk™ | NECsociety
I just asked our Nicu nurse about why we couldn’t room in with our babies since we have a private room for my son. I guess the dept of health requires a bathroom in room if a person stays the night.
Pingback: The Roller Coaster of Breastfeeding in the NICU - Preemie Babies 101
Pingback: Our Frustrating NICU Experience - Humble in a Heartbeat
Pingback: Breastfeeding in the NICU – Micronutrients and More - Breastfeeding Tips and Breast Pump Info for Moms from Medela Canada
Pingback: Moby Wrap Giveaway! | NECsociety
I delivered at Cedars-Sinai in Los Angeles and the support was pretty good. They were adamant about the need to pump for my 30 weeker and we started breastfeeding at 32 weeks with the help of lactation consultants. Comfy chairs and privacy screens were provided and there is a lactation room for pumping. My baby came home at 35 weeks and is exclusively breastfed. We never needed a shield. We could have gone home a week earlier except for apneas and bradys. My only complaint is that there was nowhere in the NICU to nap/sleep at night. That would have made a lot of difference.