 This post is the 43rd in a series on the Booby Traps, made possible by the generous support of Motherlove Herbal Company.
This post is the 43rd in a series on the Booby Traps, made possible by the generous support of Motherlove Herbal Company.
In a prior post I discussed a number of barriers to breastfeeding many moms encounter in the NICU. While many NICUs have a long way to go in supporting breastfeeding, there are some which have made great strides in implementing policies and supports which make breastfeeding and breastmilk feeding a reality for moms and babies.
I’m thrilled to be able to share an interview with Dr. Diane Spatz of the Children’s Hospital of Philadelphia about how she changed her own NICU, her “Ten Steps for Promoting and Protecting Breastfeeding for Vulnerable Infant,” and her own advice for beating the Booby Traps in the NICU.
Dr. Spatz is Associate Professor of Health Care of Women and Childbearing Nursing and Helen M. Shearer Term Associate Professor of Nutrition at the University of Pennsylvania. She holds a joint appointment at The Children’s Hospital of Philadelphia (CHOP) as a nurse researcher in lactation. Her expertise is the provision of human milk/breastfeeding in mothers who have infants with complex surgical anomalies. Dr. Spatz is a Fellow in the American Academy of Nursing (AAN) and is Chair of the Expert Panel on Breastfeeding for the AAN.
What are some of the reasons why moms experience the NICU Booby Traps I described in a prior post? Which of these issues do you see changing for the better in NICUs these days?
One of the primary barriers to the use of human milk and breastfeeding in the U.S. is not viewing human milk as an intervention that changes health outcomes. Far too many health professionals assume that mothers have the necessary information needed to make an informed decision. This is not true! For mothers expecting an infant in the NICU or other critical care unit, mothers must be presented with the science of human milk. Human milk must be viewed as a medical intervention that is just as important as IV nutrition or a ventilator.
 At the Children’s Hospital of Philadelphia (CHOP), we have a prenatal lactation consultation that occurs as a standard part of prenatal care. All mothers are informed with tailored information as to why their milk is essential for their infant. This has resulted in a 99% pumping initiation rate in our Special Delivery Unit (SDU). If you present moms with the research about why their milk matters and how human milk works to protect their infant from disease and illness, all moms want to pump! Moms want to do what is best for their infants.
At the Children’s Hospital of Philadelphia (CHOP), we have a prenatal lactation consultation that occurs as a standard part of prenatal care. All mothers are informed with tailored information as to why their milk is essential for their infant. This has resulted in a 99% pumping initiation rate in our Special Delivery Unit (SDU). If you present moms with the research about why their milk matters and how human milk works to protect their infant from disease and illness, all moms want to pump! Moms want to do what is best for their infants.
The second barrier to breastfeeding and human milk in the NICU is a lack of evidence-based lactation support. Every single barrier you mention could be solved if the administration and all health care providers read and understand the evidence. I will argue that nurses are the KEY to success, yet nurses routinely are NOT educated about breastfeeding and human milk in their programs of study, or if they are the information is minimal. At the University of Pennsylvania, I teach an entire semester undergraduate course to nursing students. This course provides future nurses with 28 hours of lecture and 14 hours of clinical exposure!
Can you describe the process of change to more breastfeeding-friendly practices in your NICU at The Children’s Hospital of Philadelphia?
Prior to being recruited to CHOP, I had always worked at birth hospitals. In that setting there is a lot of access to mothers and opportunities for education, even though they stay for a short time. I was also shocked when I saw the lack of knowledge about breastfeeding (even though this exists in ALL hospitals), and that the mindset was about taking care of the infants, forgetting that moms = the food supply for the babies! So I knew I had some big issues to address. I needed to create a culture in which human milk was valued as a critical intervention for NICU infants.
Data is KEY! Hospitals must collect and track data on their breastfeeding practices. One of the first things I did was take pictures of all of our human milk storage areas (which identified issues to resolve). The next was to do a basic knowledge assessment of staff, followed by a survey of pump room usage. You cannot just say you have a problem without identifying what the problem is!
The key driver in changing our breastfeeding culture at CHOP is our nursing staff. Our nurses take a two-day, 16 hour Breastfeeding Resource Nurse Course. This class is a job requirement of all NICU nurses. Over 650 nurses have completed this course, and there is a refresher course that nurses take every 2 years. In addition, CHOP has a hospital-wide breastfeeding committee with unit-based champions in every patient care area. Every month, we meet to discuss human milk and breastfeeding concerns, and our mission is to always focus on how we can do better and our serve our families better.
Every organization should treat themselves as an unfinished prototype and continually strive to improve their breastfeeding culture. This cultural change cannot be done by one person; all members of the organization must be educated as to how they play a role in the protection and promotion of human milk and breastfeeding. Nurses are the KEY!
You have written your own Ten Steps for Promoting and Protecting Breastfeeding for Vulnerable Infants. Can you describe them?
Step 1-Informed Decision Making. All moms must be presented with the science and the evidence about why and how human milk will help their children have better health outcomes. The ideal time for this evidence to be presented is prior to delivery. However, if this did not occur prior to admission to the NICU, the mom should be presented with the evidence showing that human milk is the only thing that should be put in a NICU infant’s stomach. This also means that the institution should have donor milk available!
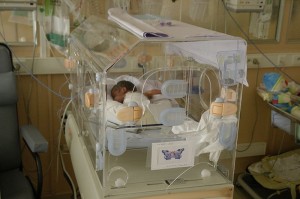
NICU image courtesy Wikimedia Commons
Step 2-Initiation and Maintenance of Milk Supply. Mothers rarely receive evidence-based guidance related to pumping initiation. A healthy term infant would breastfeed immediately (within the first 1-2 hours for sure), yet mothers who have infants admitted to the NICU often are not counseled about early and frequent milk expression with a high quality hospital grade pump. It is absolutely essential that moms with NICU infants mimic what healthy term infants would do at the breast. At CHOP, we have actually conducted a continuous quality improvement project to ensure that all of our moms in the SDU are pumping within 2 hours of a vaginal delivery, and within 4 hours of a cesarean. It is essential for moms to pump early and frequently! Healthy term infants feed on average 11/breasts per day (Range 6-19), therefore a mom has to pump every 2-3 hours with a goal of 8 pumps in a 24 hour period.
Tracking milk production is essential. Unfortunately in the NICU, the infant may be NPO [nothing by mouth] for a long period of time and therefore no one is monitoring maternal milk supply. It is essential for moms to track their daily pumping and milk supply. Moms should be given the goal of pumping 8 times per day and achieving a supply of at least 500-1,000 milliliters by the end of the first week. Moms should be tracking their milk production in a pump log (paper or electronic), so that any milk supply concerns can be addressed early on. Hospital grade breast pumps are essential for pump-dependent moms. Unfortunately insurance reimbursement for pumps is lacking. Many mothers must pay out of pocket for the cost of a hospital grade pump. Moms should speak with their insurance and/or the WIC program about pump provisions. Moms can also ask if their hospital has a pump loan program. In addition, shield fit is critical (the part that attaches to the breast). If the shield is too small (or too big) milk ejection and emptying of the milk can be comprised and nipple damage can also occur. The nipple should be observed before, during, and after pumping to ensure that it is not getting “stuck” in the tunnel of the shield.
Step 3-Human Milk Management. Hospitals should provide adequate refrigerators and freezers in which moms store their milk. The hospital should have in place a system to ensure that the right infant receives the right milk. (For example, a two health care provider check or a scanner system). In addition, how milk is fed is critical. Colostrum should always be used to initiate enteral feeds (feeds in the gut). Colostrum should be fed for 48-96 hours in the exact order that mom pumped the milk. At CHOP, we use an orange dot system and moms number the colostrum. Colostrum is stored in special containers and in a separate bin. Once the infant’s gut is primed with colostrum, then fresh milk should be fed. Fresh milk is milk that is pumped at bedside or milk that has only been refrigerated. Milk can be stored in the refrigerator for up to 96 hours. Some NICUs will freeze milk to kill CMV (a virus), however freezing milk does not kill CMV and it destroys many beneficial components of human milk.
Step 4-Feeding of Human Milk and Lacto-engineering. Prior to initiation of enteral feeds (feeds in the gut), and during the whole time the infant is NPO, the infant should receive oral care with both colostrum and/or mature milk. Oral care should be done ideally each time mom pumps at the bedside. A sterile swab can be used to coat the inside of the baby’s cheeks with the milk.
Once the infant can get feeds, colostrum should be fed first, and then fresh milk. Fresh milk contains live white blood cells and the maximum potency of immune-biological components.
Access to donor milk is also still a huge barrier in NICU care. Moms own milk is always the best intervention. If the mom is experiencing a low milk supply or delay in the establishment of milk supply, donor milk should be available (see the 2012 American Academy of Pediatric new policy statement). Many hospitals cite cost as the problem, however the cost of donor milk is minimal, especially when compared to total parental IV nutrition.
Human milk is highly variable. The nutrient content of human milk is enhanced when an infant is born preterm (more fat, protein and carbohydrates). The fat content in human milk changes from the beginning of a pump/feed to the end of a pump/feed. In addition, how full/empty a breast is will change caloric density. For example, the first pump in the morning (after a longer rest at night) will result in fuller breasts and lower fat content milk.
Moms can easily be taught how to fractionate their milk. Moms can separate their fore milk from their hind milk. This allows the infant to get more fat and calories, and to achieve better growth.
Step 5-Skin-to-Skin Contact. Skin-to-skin is absolutely magical! Ask every day, “When can I hold my baby skin to skin?” Hold you infant skin-to-skin for as many hours per day as you can. Pump first, hold your baby and then pump after skin-to-skin. Babies who are intubated and have IV lines can and should be held skin-to-skin!
Step 6-Non-nutritive sucking (NNS). As soon as your baby is extubated, he/she should start non-nutritive sucking at the breast. If the baby was not intubated, the baby should do NNS from birth. If the hospital staff is worried about the baby transferring milk, the mom should be advised to pump first. NNS allows the baby to practice breastfeeding before he/she has to perform. Many moms are worried about pacifiers in the NICU. Pacifiers are good for growth, development, organization, sucking skills. However, pacifiers should be used when you are not there! If you are in the NICU, your breast is the original pacifier.
Step 7-Transition to breast. Ask your nurse every day if your baby is ready to breastfeed. There is no research indicating that a baby must bottle-feed before it can breastfeed. It is crucial for you to be your own advocate. This means mom must be in the NICU frequently to breastfeed. Don’t expect the baby to transfer much milk on initial breastfeeding attempts. This is normal. Ask your nurse for the opportunity to do maximal breastfeeding before introducing the bottle. Nipple shields can facilitate breastfeeding and milk transfer for the NICU infant.
Step 8-Measuring milk transfer. Pre- and post-weights (also called test weights) allow us to know exactly how much the baby takes from the breast. A very precise scale must be used. The scale should be accurate to +/- 2 grams. We use the Baby Weigh® scale at CHOP. By doing pre- and post-weights, you will know exactly how much the baby is getting from the breast and prevent over or under feeding.
It is absolutely essential that the baby is weighed in the exact same conditions before and after the feed. This means that you cannot change the baby’s clothing or diaper. All leads must be disconnected and put on the scale (not held up in the air). Precision in technique is critical.
Step 9-Preparation for Discharge. Ask the nurse to be able to stay all day or all night and feed the baby on cue or on demand. The baby may breastfeed every 1-3 hours. This is normal. Pre- and post-weights will allow you to know what the baby is taking in. You will need to continue to pump during this period. The pump must be the driver of your milk supply until the baby is effective and efficient at taking all feeds completely from the breast!
Step 10- Access to Health Provider who is Knowledgeable about Breastfeeding a NICU Baby. Many health care providers do not receive lactation/breastfeeding education. For the NICU graduate, moms will likely need to continue to pump at home to maintain supply as baby is learning to breastfeed. Mom should be advised to rent a Baby Weigh® scale at home to measure milk transfer. Most NICU babies are not efficient at breastfeeding until at least 2 weeks after mom’s due date.
Be patient! Your hard work of pumping and breastfeeding will pay off! You are making an investment in your child’s future. It will get easier. Take advantage of breastfeeding support groups or organizations in your community!
Also remember that when you return to work, [many moms] are entitled by law to be given time and space (that is not a bathroom) to express milk at work!
Knowing what you do about how NICUs work, if you were a NICU mom who wanted support for breastfeeding and breastmilk feeding but weren’t receiving it, what would you do?
- Do your own research
- Advocate for your baby
- Be at your baby’s bedside
- Visit as many hours a day as you can
- Pump at your baby’s bedside
- Talk to your nurses every day about doing oral care
- Talk to your nurses every day about when the baby can be held skin-to-skin
- Once the baby is extubated (if he/she was), ask your nurse every day when you can start non-nutritive sucking at the breast.
- Tell your nurse you want to be able to put the baby to breast before he/she gets a bottle
- Breastfeed as many times a day as possible
- Use a scale to weigh the baby before and after feeds to know how much the baby takes
- Ask the nurse if you can room-in all day or all night to breastfeed
- Remember, you are the mom! This is your baby! Ask the staff to help you achieve your personal breastfeeding goals!













I would be interested in knowing when Dr. Spatz instituted these changes. My son spent 6 weeks in the CICU and NICU at CHOP 5 years ago, and I was never afforded any of these opportunities. I was loaned a hospital grade pump with no instructions, and after 4 weeks I was finally told I could pump at his bedside. They refrigerated what (very) little milk I could get when I pumped at home or the pump rooms, but by the time he was ready for ng feeds, there was hardly anything to give him and they went immediately to formula. Only one single time did a nurse offer to help me and only one time did a nurse allow me to try non-nutritive suckling. The result of this, of course, was that at 5 weeks, I was almost completely dried up without ever having a real chance at nursing him. This was devastating to me, but at the time I had no idea that I should have been given a better chance to accomplish it. In fact, this article is what has made me realize that I could have had a better chance. I love CHOP and their nurses, but this article has really brought up a sore subject for me and now I know that all of the hurt I endured may have been prevented.
I had my baby at CHOP two years ago (born there) and in the NICU for over 3 months. Diane is my hero. Everything in this article is true. She is AMAZING. I pumped for a full year thanks to all of the support that I was given. I have no doubt that this helped my little girl survive. She’s doing very well now. I love this article! Thank you.
What is the best way for a mother with a baby in the NICU who is facing unsuitable protocols and uncooperative nursing staff and/or neonatologists who do not follow evidence based practices?
Whoo Hoo! I am in the Philadelphia region and have known for years about the great work (and tireless publishing …) of Diane Spatz. Nursing (as in RN-nursing) and nursing (as in breastfeeding-nursing) are fortunate to have this researcher and lactation advocate. P.S. she wrote, along with another Philly star Rachelle Lessen, ILCA’s great evidence-based paper “Risks of Not Breastfeeding.”
My daughter was born at CHOP 3 years ago and Diane was amazing!!! She taught me so much!!! She was so supportive as were all the nurses!!! Even after I was discharged Diane still helped me with any questions I had!!! I was able to give my daughter beast milk for a year!!
It is very true how little people know about breast feeding even medical professionals!!! The world should have more people like Diane and the nurses at CHOP!!!
My son was born at UMMC (Jackson,MS) 4 years ago. I wish we had even a few of these going when we were there. In the 5 days before my son was born I went on an info hunt. I was given 0 hope for his survival due to the severity of his case (27w 590g Blue ToF) and was adamant on finding anything increase his chances. Breast milk, of course, being one. So I pushed for a pump and pushed for only using my milk. They did used fortifier packets, and if I had realized what it really was and that I made such high cal milk (31.5 ) I would have not let them use it. After we left the Neonatoligist was able to use our case to FINALLY get donor milk and all micros get it now. The hospital is also now on the path to become “baby friendly”. Not bad for a little boy who would be lucky to survive birth and at best wouldn’t live 2 weeks. He is 4 years old next month.
A suggestion to add to this list: passifiers should be used when starting a tube feed so that they get used to sucking and the stomach filling. After 5.5 months in the NICU and 5 months of that totally tube fed, he has almost 0 oral aversion. He doesn’t like chicken nuggets and is just now starting to eat a bit of ice cream (hates cold).
Pingback: FAST FACTS: Miracle Milk™ | NECsociety
Pingback: When Will My Milk Come In? - The First Latch | Lactation Info, Education, and Support | Breastfeeding | Brooklyn NYC